Colorectal cancer is one of the leading causes of death in the United States. In fact, research shows that it is the third-leading cause of cancer-related death in the United States, will result in over 53,000 fatalities in 2020, and will appear in almost 150,000 patients over that same time frame.
As with many health issues, knowledge of colorectal cancer means power: the power of early detection, treatment, and in some cases even prevention. You may worry that you or a loved one are at risk for developing colorectal cancer; or you may want to better understand certain aspects of this disease. If so, then the following information will likely prove to be very helpful to you, as it covers several frequently asked questions about this type of cancer.
What is Colorectal Cancer?
Colorectal cancer is a cancer that starts in the colon or rectum (the last part of the digestive tract).
It is important to note that the term “colorectal cancer” is actually a combination of colon cancer and rectal cancer. Colon cancer can start anywhere in the colon, whereas rectal cancer is confined to the rectum, or the last 5 inches of the colon. However, since these two cancers target the same general region of the body, they are usually referred to by the single phrase “colorectal cancer.”
What is the Colon?
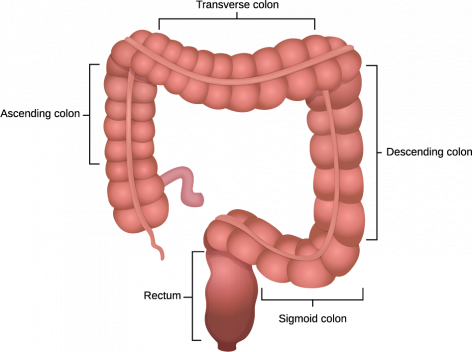
The colon, also known as the large intestine, is a tube-like structure designed to remove fluid and salt nutrients from waste, temporarily store that waste, and then finally push it out of the body. Your colon is shaped like a little “n” with an entryway that connected to the small intestine and a discharge section (the rectum) that finally eliminates waste when you have a bowel movement. It has 5 basic parts:
- The ascending colon
- The transverse colon
- The descending colon
- The sigmoid colon
- The rectum
How Does Colorectal Cancer Develop?
The majority of colorectal cancers start out as a polyp, or a small growth with a stalk that protrudes from the inner lining of the colon or rectal wall. There are two common kinds of polyps:
- Hyperplastic polyps. These are usually benign and occur in areas where your body has repaired damaged tissue.
- Adenomas. These polyps are generally considered pre-cancerous. Anywhere from one-third to one-half of people will develop at least one adenoma which, if not removed, could become cancerous over the course of 5 to 10 years.
What are the Signs and Symptoms of Colorectal Cancer?
One of the most daunting aspects of colorectal cancer is the fact that its symptoms may not appear until after the cancer has already progressed and spread. In addition, many common signs of colorectal cancer are the same symptoms that arise from less dangerous conditions, such as hemorrhoids or irritable bowel syndrome (IBS).
Symptoms of colorectal cancer may include:
- Diarrhea, constipation, or narrowing of the stool (e.g. stool that is stringy or pencil-like) that lasts for several days
- The sensation that you need to have a bowel movement even after you have one
- Rectal bleeding
- Blood in the stool, or extremely dark stool
- Abdominal cramps
- Fatigue
- Unintended or sudden weight loss
Is Colorectal Cancer Hereditary?
Only 5% or so of colorectal cancers are considered to be hereditary. However, if close relatives such as parents, siblings, or children have been diagnosed with colorectal cancer, then your odds of also developing this cancer are 2 to 3 times higher than the average person.
5% of colorectal cancers are hereditaryIn addition, certain inherited conditions can increase the risk that you will develop colorectal cancer. These include Lynch syndrome and Familial adenomatous polyposis.
What is a Screening Colonoscopy, and When Should I Have One?
A screening colonoscopy is an outpatient procedure that is performed on sedated patients. In this procedure, a flexible scope equipped with a lighted camera is used to inspect the entire colon and rectum. During the operation, the surgeon will generally remove any polyps discovered in the colon. In order to prepare for the colonoscopy, the patient is typically instructed to only drink clear liquids like water and chicken broth the day before the procedure.
It is generally recommended that patients with an average risk of colorectal cancer should begin screening at 45 and (if no concerns are raised) to do so every 10 years thereafter. Of course, there are some exceptions to this guideline. For instance:
- African Americans are usually at higher risk for colorectal cancer, and should thus begin screening earlier than age 45
- Individuals with a family history of colorectal cancer should begin screening around age 40
- Any other individuals at high risk (those with hereditary syndromes, IBS, etc.) should begin screening earlier than age 45, and should screen more frequently thereafter
Are There Other Ways to Detect Colorectal Cancer?
There are some alternative screening options besides the traditional colonoscopy. These include:
- Flex sigmoidoscopy
- Virtual colonoscopy
- Stool testing
In the near future, researchers may also develop a blood test for colorectal cancer detection. It should be noted that if any of these tests come up positive for colorectal cancer markers, it is most likely that your attending physician will still recommend a traditional colonoscopy.
What is the Prognosis When Diagnosed with Colorectal Cancer?
The 5-year overall survival rate for patients diagnosed with colorectal cancer, regardless of the stage, is about 65%. When individuals are diagnosed with the disease in its early stages, that rate shoots up to 90%.
As of this writing, less than 65% of individuals over the age of 50 have had some form of colorectal screening. The National Colorectal Cancer Roundtable has the stated goal to drive that percentage up to 80%, which could prevent over 200,000 deaths within the next two decades.
Colorectal screening can save lives but only if people get screened. The best test is the one you will do.
Can I Prevent Colorectal Cancer?
There is no 100% guaranteed way to prevent colorectal cancer. Nevertheless, there are several things that you can do to reduce your risk of developing this disease. These include:
- Engaging in 2 1/2 hours of moderate to strenuous physical exercise every week
- Taking in adequate amounts of calcium, fiber, fruits and vegetables
- Reducing your intake of red and processed meats
- Limiting daily alcohol consumption (1 drink for women, 2 drinks for men)
- Avoiding/quitting cigarettes and other forms of smoking
- Working to maintain a healthy body mass index and weight
Even though colorectal cancer can be a scary prospect for many, if you know your family’s medical history, screen early, and cultivate a healthy lifestyle, then you will greatly reduce your risk of developing this harmful disease.
Arizona Oncology plays a major role in helping people throughout the state, and their families, win their battle against colorectal cancer by providing easy access to a full range of advanced cancer care services in a setting that allows patients to remain close to their homes and their support network of family and friends.
Originally written February 2018. Updated February 2020.




